Addressing those ‘windy days’ – effective diet and treatment options

 The taboo topic
The taboo topic
There is a common consensus that passing wind or farting is embarrassing and unpleasant. The noise, odour and overall concept almost make our toes curl and is the butt of many jokes ew, eurgh, gross…
But, have you ever thought of farting as something good, positive or even something to be proud of? You might be surprised to know that there are some cultures that see farting in a positive light. For example, men from the Pira-Parana area of the North-West Amazon delight in farting loudly, and apparently modulate the noise with their fingers or cupped hands. If that’s something you’ve never heard of then how about Le Pétomane? Joseph Pujol, more commonly known by his stage name Le Pétomane, was a French flatulist and entertainer who was famous for his talent in farting. In other words, he was a professional farter.
Whether you refer to it as farting, passing wind, or flatulence, it is a normal biological process which everyone experiences on a daily basis.
The facts
Flatulence is a medical term to describe releasing gas from the digestive track through the back passage. It is completely normal – if anything it would be unusual to never pass wind. There is no medical guidance on what the normal frequency or volume of flatulence should be, but the average frequency varies from 5-15 times a day. The normal volume is between around 500 to 1500 mls and some might be surprised that it is equal in men and women. The offence is arguably more the consequent of living indoors rather roaming the plains, as perhaps nature intended.
 Causes
Causes
There are many reasons why we pass excessive amounts of wind. Some people may just do so naturally. However other causes can be excessive air swallowing (aerophagia), which is a common cause of frequent burping. You may not realise but during chewing or any mechanical movement of the mouth, we are swallowing small amounts of air. These small amounts of gas eventually build up in the digestive system and are released as wind.
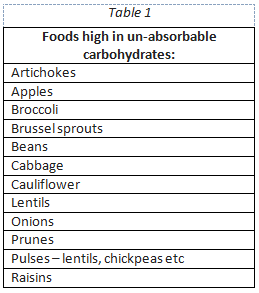
Flatulence can also be related to eating foods which are difficult to digest and as a by-product of fermentation by the gut microbiome (GM) in the large intestine. For instance, foods high in un-absorbable carbohydrate (also known as fibre) are passed down to the large intestine (colon) to be broken down by the bacteria which produce gas (see Table 1 for a list of foods which are high in poorly absorbed carbohydrate).
If you are unable to digest specific foods and have a food intolerance to lactose or wheat for example, this can result in a similar change occurring in the large intestine. Passing wind is also a common symptom in many gastrointestinal conditions such as, irritable bowel syndrome (IBS), lactose intolerance, coeliac disease, small intestinal bowel overgrowth (SIBO), gastroenteritis and indigestion. A clear diagnosis and treatment of any underlying conditions is clearly important in managing the condition. If the symptoms are mild and long standing, it is often not necessary to undergo any tests, particularly if simple measures control the condition adequately.
You can contact your GP for a referral to have a consultation with Andrew if your flatulence is excessive and interfering with your work and/or social life, click here for more information. Otherwise, keep reading for some tips to try beforehand!
How to reduce flatulence
As mentioned earlier, passing wind is a normal action and it may be best to manage the ‘where and when’ rather than trying to reduce the volume or frequency. However, there are ways to control the amount of wind you pass if you experience excessive flatulence. Have a scroll through the different things you can try, below.
 Avoid or reduce intake of foods which are prone to be gaseous.
Avoid or reduce intake of foods which are prone to be gaseous.
High fibre foods are generally healthy and should form an important part of a healthy and balanced diet. However, reducing intake of foods high in certain fibres (see Table 1) may help your body pass less wind. Other foods which are less healthy include artificial sweeteners, fizzy drinks, sugar-free sweets or chewing gum. A two-week trial of avoidance can help to identify which foods and drinks might be causing the problem. But remember to not restrict yourself from a healthy and balanced diet. A high fibre diet is also good in maintaining a healthy gut microbiome.
- Eat and drink more slowly.
This is a crucial one. Our body is like a factory. The mouth is the entrance to the long corridor of the gastrointestinal tract. Rapid eating is likely to promote air swallowing which will contribute to intestinal gas. Eating slowly also contributes to the brain being satisfied (food satiety) which helps us to avoid getting hungry too soon and thus helps avoid obesity.
- Eating little and often.
Eating smaller and frequent meals allows the body to digest a small amount at a time. This reduces the chances of passing an excess amount of wind. You can do this by splitting 3 main meals a day into 6 small meals a day.
 Exercise regularly.
Exercise regularly.
Our bodies can be viewed as a sort of factory. This factory needs to be maintained! This involves moving the parts around (exercising) to ensure they don’t get rusty or slow. The UK physical activity guideline recommends at least 150 mins per week. This can be broken down and spread to a minimum of only 30 minutes on 5 or more days each week.
- Peppermint tea. There is also some evidence to suggest that peppermint tea helps gut digestion and the symptoms of flatulence. Swapping a cup of coffee or other tea for peppermint tea in your day may be worth a try.
- Probiotics – may also be useful in treating flatulence particularly if you have Irritable Bowel Syndrome. We have an informative blog on this subject: click here.
- Some medications increase wind including NSAIDS such as ibuprofen. It may be worth reviewing the information on side-effects on any treatment that you are taking. Always discuss changes in your medication with your doctor if at all possible.
- Simethicone is used for wind in babies and can help adults too; this can be easily purchased from your local pharmacy.
- Activated charcoal has also been shown to help in reducing wind and can be bought from pharmacies and other outlets.
- There are many other preparations, supplements and digestive enzymes that are reported to help but have less scientific evidence that they work.
- Pharmacists are often experienced in advising patients on conditions such as wind and your local Pharmacy should be able to offer you good advice on managing the condition.
If your symptoms persist, it is a good idea to go and discuss your symptoms with your doctor.
At BeGoodToYourGut we have a great team who specialise in gastrointestinal issues. If you would like to be seen by either a Consultant Gastroenterologist and Hepatologist Dr Andrew Millar and Gastroenterology Specialist Dietitian Sian Shepherd then be sure to click here.
This blog was written by Student Dietitian Sena Ali and edited by Sian Shepherd (Specialist Gastroenterology Dietitian) and Dr Andrew Miller (Consultant Gastroenterologist).
Tags: abdominal pain, activated charcoal, Bloating, dietitian, digestion, Digestive Health, Flatulence, Gut microbiome, IBS, IBS symptoms, Irritable Bowel Syndrome, probiotics, windy foods
0 Comment
Leave a Reply